Uncategorized
Prescription Delivery Near Me: A 2026 How-To Guide
You're probably here because a prescription is ready, or almost ready, and getting to the pharmacy feels harder than it should. Maybe you're sick, caring for someone else, working around a packed schedule, or trying to stay on top of a chronic condition without adding another errand. In those moments, searching prescription delivery near me makes sense.
Delivery can make treatment easier to start and easier to stay on. But the first result on a map isn't always the right fit. That matters even more if your medication needs refrigeration, prior authorization, pharmacist follow-up, Medicaid billing, or extra handling because it's a controlled or specialty medication.
Use delivery as a healthcare decision, not just a convenience decision. By 2022, 46% of patients had used a prescription delivery service, yet only 24% used delivery as their primary method, even though 52% said they preferred delivery over in-store pickup, according to RxSS reporting on prescription delivery adoption. That gap tells me many patients want delivery, but still run into barriers when they try to use it in real life.
Table of Contents
- Your Guide to Prescription Delivery in 2026
- How to Find Reliable Prescription Delivery Services
- Verifying Insurance and Specialty Medication Coverage
- Preparing and Submitting Your Prescription for Delivery
- Comparing Delivery Models Timelines and Costs
- Staying Safe and Protecting Your Privacy
- Making Prescription Delivery Work for You
Your Guide to Prescription Delivery in 2026
A local search is a starting point. It isn't a decision by itself.
When patients search for prescription delivery, they usually find three types of options: a nearby retail pharmacy with in-house delivery, a chain pharmacy that uses a courier, or an online or specialty pharmacy that ships directly. All three can work. They just don't work equally well for every medication.
Start with the pharmacy, not the app
If you already have a prescription on file, call the pharmacy that currently fills it and ask a narrow set of questions. Do they deliver your exact medication. Do they bill your insurance for delivery orders. Can they handle signature requirements, refrigeration, or refill coordination. A fast answer tells you a lot about how organized that service is.
If you're starting from scratch, search by your medication type as well as location. “Prescription delivery near me” is fine for an antibiotic or maintenance blood pressure medication. It's less helpful for a GLP-1, hormone therapy, ADHD medication, or any drug that triggers plan restrictions.
Practical rule: Match the delivery model to the medication. Common medications can often go through local delivery. Complex therapies usually need a pharmacy that handles benefits, refill timing, counseling, and specialized packaging.
Use a short vetting checklist
Before you move a prescription, check these basics:
- Real pharmacy identity: The site should clearly name the pharmacy, list a phone number, and identify where pharmacist help is available.
- Clear delivery rules: Look for written details on service area, signature needs, missed deliveries, temperature-sensitive items, and transfer requests.
- Medication-specific answers: If the FAQ only says “free delivery” and nothing about insurance, controlled prescriptions, or specialty drugs, expect friction later.
- Accessible pharmacist support: Delivery works better when you can still ask counseling questions before the package leaves.
A nearby option can be convenient. A suitable option is what keeps treatment moving. That distinction saves the most frustration.
How to Find Reliable Prescription Delivery Services
Reliability starts before the order is placed. Most patients check speed first. I'd check operational clarity first.

Where to search first
Google Maps is still useful because it shows hours, phone access, and whether a pharmacy advertises delivery at all. Major chain websites can also help because they usually spell out whether delivery is same-day, next-day, or mail-based. Third-party apps may show pharmacy delivery too, but patients often discover the hard way that app availability doesn't guarantee medication eligibility.
Reviews can help, but read them carefully. A review that says “fast service” matters less than one that mentions refill accuracy, communication about delays, or how the pharmacy handled an insurance issue.
What a trustworthy listing looks like
A reliable service usually has a consistent pattern. The pharmacy explains how prescriptions are submitted, who handles transfers, what happens if a package can't be delivered, and how to reach a pharmacist. Vague language is a warning sign.
Use this screening list when you compare options:
- Check licensure signals: Look for clear pharmacy identification and verification details, not just a delivery storefront.
- Read the delivery policy: You want specifics on hours, cutoffs, signatures, and exceptions.
- Test the phone line: Call once before sending the prescription. If you can't reach anyone, delivery problems get much harder to solve.
- Ask one medication-specific question: For example, “Can you deliver a refrigerated medication?” or “Can you bill Medicaid managed care on this order?”
A service can be close to your home and still be the wrong fit for your prescription.
Reliability matters more for complex coverage
Many local options break down at this stage. Patients with Medicaid, managed care, or specialty prescriptions often see a delivery promise online, then hit a denial, transfer delay, or “cash only” surprise after the prescription is already in motion.
That's why I tell patients to evaluate the pharmacy's ability to process the claim, not just drop off the bag. A delivery service that can't handle the plan or medication category isn't really solving the problem.
Verifying Insurance and Specialty Medication Coverage
“Free delivery” only describes transportation. It doesn't tell you whether your medication is covered, whether prior authorization is needed, or whether the pharmacy is allowed to fill that prescription under your plan.

Ask these questions before you transfer anything
For common medications, insurance verification is often straightforward. For GLP-1 therapies, hormone therapies, and other specialty medications, it usually isn't. The key is to confirm both network status and drug-level coverage before your prescription gets stuck in limbo.
Use this sequence:
- Ask whether the pharmacy is in network for your exact insurance plan.
- Ask whether your medication is on the formulary for that plan.
- Ask whether the claim needs prior authorization, step therapy, or quantity review.
- Ask whether delivery is included once the claim is approved.
- Ask who will contact your prescriber if documents are missing.
That order matters. Patients often focus on delivery first when the actual bottleneck is the claim itself.
Medicaid and managed care need a closer look
Retail delivery is often less flexible for specialty claims. A 2025 KFF analysis found that 35% of Medicaid patients face delivery denials for non-formulary specialty drugs at retail pharmacies. The same analysis notes that dedicated specialty pharmacies affiliated with managed care organizations like Centene can sync over 90% of chronic care regimens with Medicaid formularies, often with zero delivery fees, as summarized by Main Source Pharmacy's write-up of that KFF analysis.
If you're on Medicaid managed care, don't assume your neighborhood pharmacy can fill and deliver a specialty item just because it fills your routine medications. Those are often two different workflows.
What to do if your medication is more complex
GLP-1 therapies, hormone treatments, and other chronic-care medications often need more than a checkout screen. They may require benefits review, refill scheduling, storage controls, and pharmacist follow-up. One option in that category is Foundation Care's patient support services, which are built around specialty coordination rather than simple local drop-off.
Coverage first, delivery second. If the pharmacy can't process the claim correctly, same-day availability won't help.
A practical tip for first-time users: keep your insurance card, prescription information, prescriber contact details, and any denial letters in one place before you call. That cuts down on repeated callbacks and makes it easier for the pharmacy team to resolve missing information quickly.
Preparing and Submitting Your Prescription for Delivery
Once you've picked the right type of pharmacy, the next step is moving the prescription correctly. Most delivery delays happen here, not on the road.
The three main ways to submit
New electronic prescription. This is usually the cleanest method. Your prescriber sends the order directly to the pharmacy you choose. For new starts, this avoids confusion about stock, refills, and previous fill history.
Transfer from another pharmacy. This works well when you already take the medication and want ongoing delivery. Have your current bottle nearby so you can provide the prescription number, drug name, and old pharmacy contact information.
Pharmacy-initiated coordination. Some pharmacies will contact your doctor or previous pharmacy for you after you start the request. That can save time, especially if your regimen includes multiple medications.
If you want to start that process online, submit your prescription request through Foundation Care only if that pharmacy matches your coverage and medication needs.
Controlled and specialty prescriptions follow different rules
This is one of the biggest sources of confusion. Not every prescription that can be filled can also be delivered. Controlled substances, temperature-sensitive drugs, and some specialty medications often trigger separate identity, compliance, packaging, or signature requirements.
A 2025 CDC report indicates that 25% of U.S. adults on long-term controlled substances face delivery barriers. It also notes that only 15% of local delivery services typically accommodate them due to DEA regulations, while delivery of controlled prescriptions through specialty providers increased by 40% following telehealth flexibilities, according to Walgreens' prescription delivery information page.
That means a local “near me” result may be fine for a routine refill, but not for ADHD medications, certain pain therapies, or medications with restricted handling rules.
What works and what usually doesn't
What works:
- Exact pharmacy selection by the prescriber: Ask your clinic to send the prescription to the delivery pharmacy you confirmed, not just the nearest location in its system.
- One medication list: Include every current medication so the pharmacist can spot interactions or duplicate therapy.
- Early refill planning: Don't wait until the last dose if the medication has extra review requirements.
What usually doesn't:
- Assuming every location in a chain offers the same delivery services
- Requesting a transfer without checking whether the new pharmacy can bill the claim
- Using an on-demand courier for a medication that needs pharmacist coordination or temperature control
If your medication has any special handling requirement, ask about that first. It's the fastest way to avoid a failed handoff.
Comparing Delivery Models Timelines and Costs
Not all prescription delivery works the same way. Patients often compare by speed alone, but the better comparison is speed, fit, and how much pharmacy support stays attached to the order.
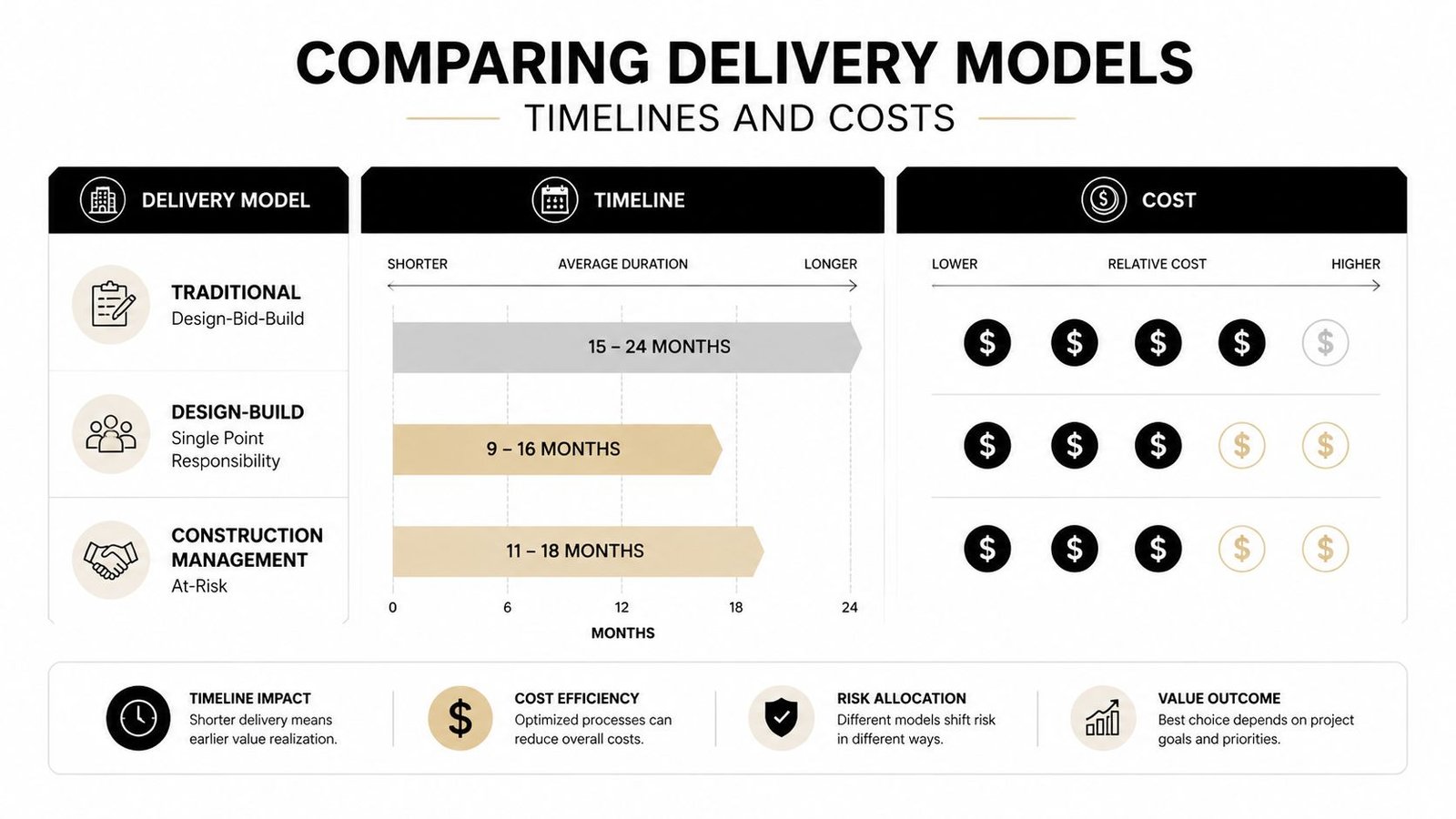
What each model is designed to do
Local pharmacy same-day delivery works well for straightforward prescriptions that are already filled, paid, and ready to leave the store. On-demand courier models are useful when a pharmacy partners with a delivery network for short-distance drop-off. National specialty or mail-based delivery is usually slower at the front end, but better equipped for chronic and high-touch therapies.
Here's a simple side-by-side view:
| Prescription Delivery Service Comparison | ||||
|---|---|---|---|---|
| Delivery Model | Best For | Typical Speed | Specialty/Cold-Chain | Insurance Handling |
| Local pharmacy same-day | Common maintenance or acute medications | Same day or next day | Limited, varies by location | Basic plan handling, varies |
| On-demand courier service | Short-distance delivery after a fill is complete | Same day | Usually limited | Often depends on the filling pharmacy |
| National specialty mail-order | Chronic, specialty, managed care, or restricted workflows | Scheduled shipping or coordinated delivery | Better suited for special handling | Stronger benefit coordination |
Reliability changes the real cost
Even when delivery is offered, patients still need the medication to arrive on time and in usable condition. A 2020 survey found that one in four mail-order users experienced delivery delays, and reliable delivery is associated with better medication adherence, better health outcomes, and reduced overall healthcare costs, according to Uber Health's prescription delivery overview.
That's why I advise patients to weigh the hidden costs of the wrong model. A delayed refill can mean missed doses, extra calls, and urgent rescue fills at another pharmacy.
Fastest isn't always safest for a complex prescription. The right model is the one that keeps the medication covered, accurate, and on schedule.
How to choose based on your situation
Choose a local same-day option if your medication is routine, your insurance is already working there, and you don't need special storage or pharmacist follow-up.
Choose an on-demand courier arrangement if the pharmacy already has your medication filled and you mainly need transport, not care coordination.
Choose a specialty delivery model if you need claim troubleshooting, prior authorization support, refill synchronization, or tracking after shipment. If order visibility matters, use the pharmacy's tracking tools, such as Foundation Care order tracking, rather than relying on generic delivery updates alone.
Staying Safe and Protecting Your Privacy
Once a prescription is out for delivery, safety becomes practical. You need the right medication, the right patient, the right package, and a clear path to help if something looks wrong.

What to check before the package arrives
Use licensed pharmacies and verify them through your state board of pharmacy if anything about the website or phone support seems off. Read the privacy policy. A legitimate pharmacy should explain how it protects health information and how patients can reach a pharmacist.
Before the first delivery, ask how medications are packaged. Sensitive medications should arrive in secure packaging, and medications that need special storage should include clear handling instructions.
What to inspect at the door
Open the package promptly and compare the label to your prescription information. Check the patient name, medication name, strength, directions, and the physical appearance if it's a medication you've taken before.
If anything seems off, stop there and call the pharmacy before taking a dose.
- Wrong patient details: Don't open sealed medication containers further. Call immediately.
- Damaged packaging: Ask whether the medication is still safe to use, especially if it's temperature-sensitive.
- Missing counseling: Request pharmacist counseling before the first dose if the medication is new to you.
- Late delivery: Ask whether the delay affects storage, dose timing, or refill continuity.
Why pharmacist access still matters
Delivery should not remove the pharmacist from your care. In a study of home delivery services, 60.8% of users cited lack of pharmacist-patient rapport as a key drawback. The same source notes a 9% medication error rate in delivery, including wrong patient delivery at 32% and mislabeling at 25%, based on National Pharmacy Association data reported in the Jordan home medication delivery study published in PMC.
Good delivery systems don't just move a package. They keep the pharmacist reachable when a patient has a question, a concern, or a problem with the order.
That's the standard to look for. Convenience matters, but safe convenience matters more.
Making Prescription Delivery Work for You
Prescription delivery near me can solve a real problem. It can save time, reduce missed pickups, and make treatment easier to continue. But the right choice depends on more than geography.
If your prescription is routine and your local pharmacy already handles your insurance well, a nearby delivery service may be enough. If you take a GLP-1, hormone therapy, a controlled medication, or a drug that needs prior authorization or specialized handling, you'll usually need a pharmacy model built for those details.
Keep your process simple. Confirm coverage first. Confirm the medication category next. Ask how the prescription will be submitted, delivered, and supported if something changes. And don't settle for a service that can transport a prescription but can't manage it.
If you need help sorting out specialty medications, managed care coverage, or ongoing delivery support, Foundation Care Pharmacy offers resources for patients and caregivers, including medication guidance, support services, and prescription coordination options.
Built with the Outrank tool

